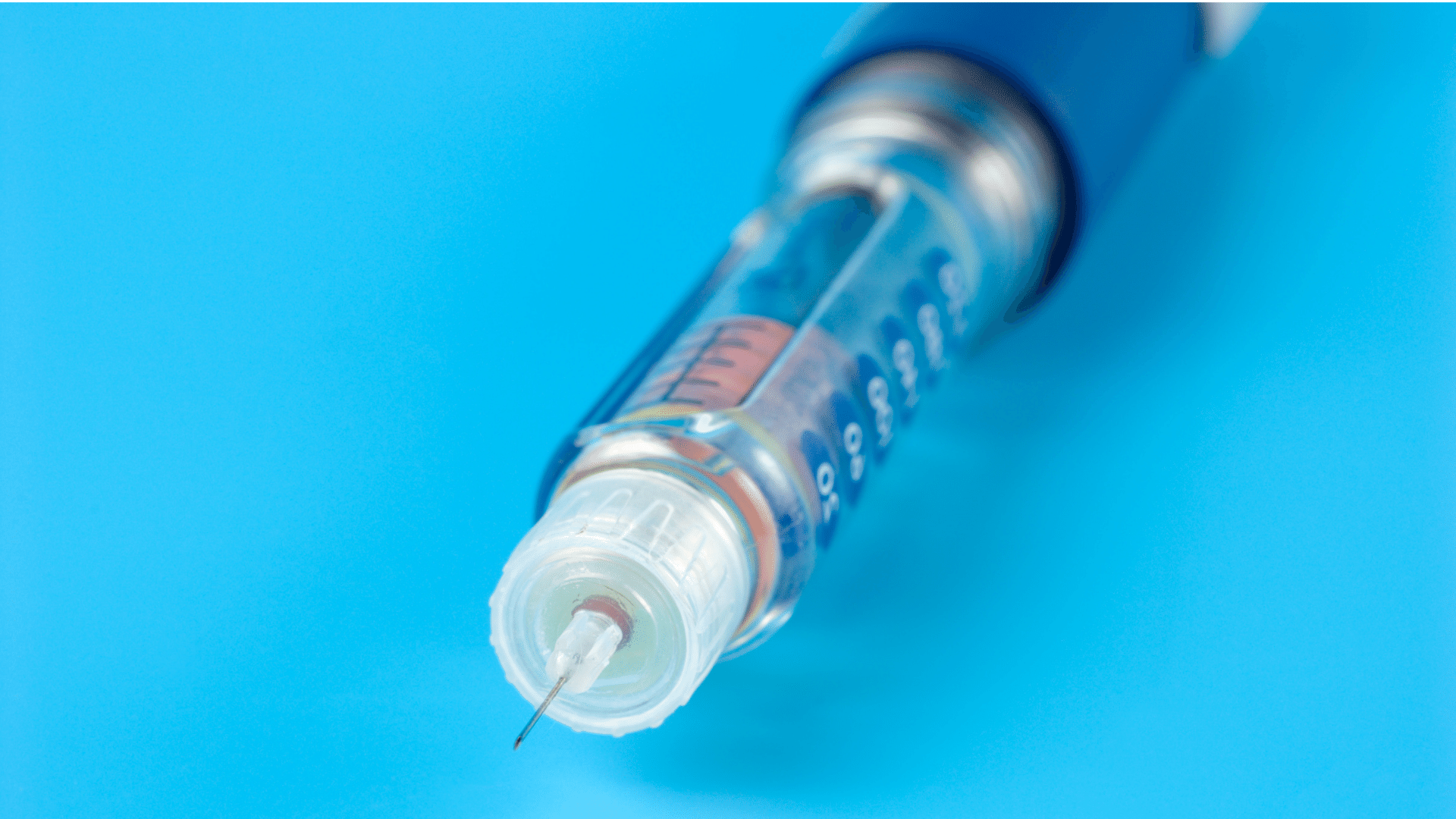
Diabetes Mellitus, more commonly known as diabetes, is a metabolic condition that causes high blood sugar. The hormone insulin moves sugar from the blood into your cells to be saved or used for energy later on.
There is a lot to be known about diabetes, however, in this article we will be focusing more specifically on insulin and the many myths that surround it.
In an ever-changing world, living with a chronic condition means that getting the right information for you or your loved one’s peace of mind is key to living a “normal” life.
Let’s take a look at some common myths and misconceptions about insulin…
I Am on Insulin Because I Have Failed to Control My Diabetes
Myth! When a healthcare provider suggests that a person with diabetes should add insulin to their oral meds, the response is normally one of disappointment. Many people living with diabetes commonly believe that switching to insulin means they have failed in some manner to manage their diabetes.
Normally, this is not the case. People with type 2 diabetes are diagnosed when their bodies lose their ability to utilise their own insulin, and the pancreas produces less and less insulin over time. A healthy lifestyle combined with oral medications may be able to keep blood sugar levels within goal limits at first.
Oral medications, on the other hand, must function in combination with the body’s own insulin to be successful. For many individuals with type 2 diabetes, the body’s own insulin supply gradually depletes to the point that oral medications are no longer effective. Insulin must then be delivered to keep blood sugar levels within a safe range.
I Am Sick, I Need to Stop Taking My Insulin
Myth! When you are sick, whether it’s a simple illness like a cold or a more serious one, your body interprets it as stress. To cope with the stress, it releases hormones that raise blood sugar levels. In some ways, this is beneficial since it helps the body get the extra fuel it requires. However, in someone with diabetes it can result in dangerously high blood sugar levels. Some illnesses have the reverse effect. Your blood sugar levels can drop dangerously low if you don’t feel like eating, are experiencing nausea or vomiting, and are taking the same dose of insulin as usual.
Insulin Injections Are Painful
You’ve never liked getting shots. They make you anxious. The sight of a needle alone is enough to make you squirm, let alone the idea of it hurting… If any of these describes you, being told you’ll have to start giving yourself a daily needle might fill you with dread.
Myth! In recent years, needle technology for diabetes medications has improved dramatically, so that the injection process is no longer as painful as it once was. There are a few things you can do to make self-injection as comfortable as possible:
- Choose the right needle. The recommendation is to use the smallest needle which is 4mm. Talk to your diabetes professional to figure out the right needle for you.
- Only use the needle once.
- Inject at a 90-degree angle, swiftly but gently. No need to go deep in skin; as long as the needle is fully in skin, no need to push further.
- Ensure that the insulin is injected at room temperature. Cold insulin may feel more uncomfortable.
Insulin Is Addictive
Myth, myth, myth! It is impossible to become addicted to insulin. Insulin is a naturally occurring hormone that your body needs! Insulin is typically present in people’s bloodstreams from birth. Diabetes, on the other hand, causes your body to produce less insulin (or none). This therapy, then, merely compensates for the insulin deficiency.
Insulin Causes Weight Gain
Myth! It’s true that many people who are given insulin gain weight. What is the reason for this? Insulin aids your body’s ability to process food more efficiently, which is a good thing! You may gain weight if you do not adjust your eating or exercise patterns appropriately. If you have any worries about this, it may help to speak with a dietician before beginning the therapy.
I Take Insulin, I Can Eat Anything I Want
Big Myth! Even if you’re on insulin, you still need to watch what you eat, just like everyone else who doesn’t have diabetes. Regularly eating excess calories can lead to weight gain in anyone, someone with diabetes or not.
It Doesn’t Matter Where I Inject My Insulin
Myth! Insulin is absorbed at different rates depending on where it is injected. It is best to use the same part of the body for each of your daily injections. However, within the specific body area, it is important to move each injection site at least one finger width away from the previous injection site to avoid the development of hard lumps or extra fat deposits, which could affect the way insulin is absorbed.
Insulin should be injected into fat beneath the skin rather than muscle, as this can result in faster insulin action and an increased chance of low blood sugar. Because of their higher fat content, the stomach, thighs, buttocks, and upper arms are popular injection sites.
Insulin Causes Hypoglycemia
Myth! The administration of an inappropriate amount of insulin will cause hypoglycemia (low blood sugar). Knowing how to properly calculate how much insulin you need is the first step in preventing hypoglycemia.
It is important to understand how hypoglycemia works and the symptoms to watch out for.
Common signs and symptoms to watch for include:
- Shakiness
- Dizziness
- Sweating
- Hunger
- Fast heartbeat
- Inability to concentrate
- Confusion
- Irritability/Moodiness
The most crucial takeaway in this section is the importance of knowing and understanding the amount of insulin appropriate for you as set out by your healthcare provider.
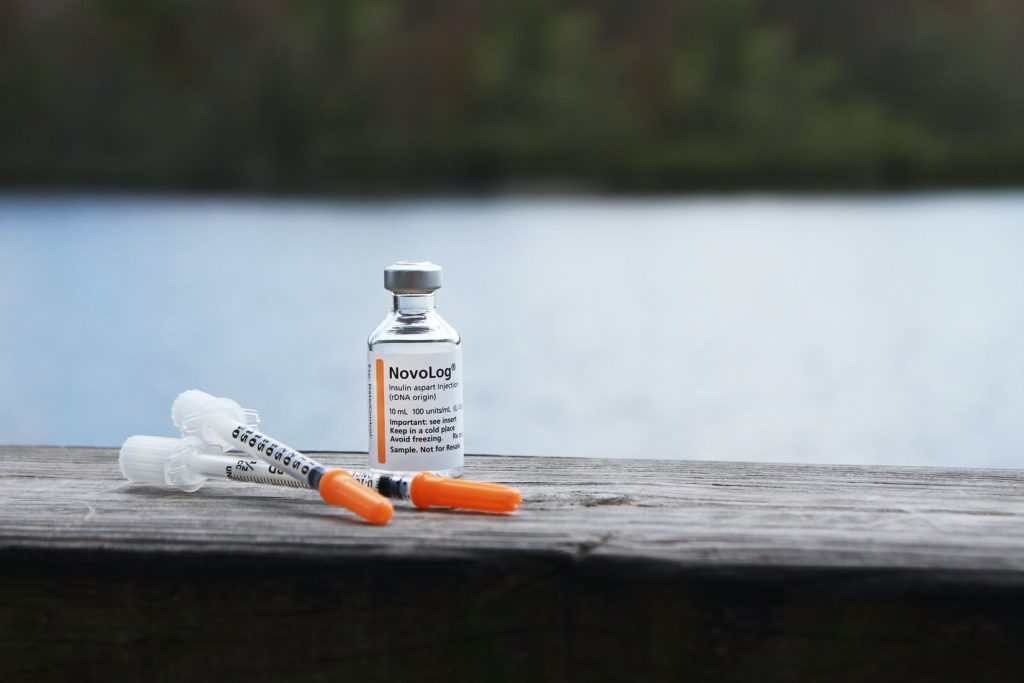
There is Only One Type of Insulin
Myth! There are numerous types of insulin products, but it is divided into these major classifications:
- Rapid-acting Insulin: Acts quickly (10 to 15 mins) and lasts 4 to 5 hours
- Intermediate-Acting Insulin: Acts slightly slower (1 to 2 hours) and lasts for 10 to 14 hours
- Long-Acting Insulin: These insulin types act slowly (1 to 2 hours) and last much longer, for up to 24 to 42 hours
- Mixtures of Insulin: Mixed short and intermediate-acting insulin divided into different amounts based on the individual case
I Can’t Go Out While on Insulin
Another Myth! Going out to eat is an enjoyable thing and having diabetes should never hinder you from doing the things you love, including eating at your favourite restaurants!
Many people are worried about the idea of taking their insulin with them when going out to eat or work since it will no longer be refrigerated.
Good news!
Did you know that rapid-acting insulin can be kept at room temperature for about 28 days? Therefore, it is perfectly safe to store your insulin with you while out-and-about. Just make sure that the insulin is not exposed to extreme temperatures and do not leave in the car.
What Is the Truth?
Starting an insulin regimen might be life-changing and frightening, but don’t be put off by social stigma, fearmongering, news articles, or websites.
Insulin is a safe and efficient therapy that millions of people with diabetes take every day. You will likely have more energy, sleep better, and have better moods if your blood sugar is well controlled. You can continue to do your normal activities, dine out, and go about your daily routine. It’s possible that you’ll need to check your blood sugar more frequently, but this will keep you safe, healthy, and informed.
You might be shocked to learn that living with diabetes is a much smaller burden than you had anticipated!